
Lumbar Facet Joint Pain: What You Need to Know (Mornington Physio Guide)
Struggling with sharp or aching pain in your lower back—worse with bending backwards, standing, or twisting? You’re dealing with lumbar facet joint pain. This guide from LivFit Physio Mornington explains what it is, how it’s diagnosed, what actuallyhelps, and when to seek help.
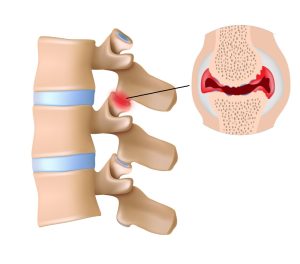
What are the facet joints?
Facet joints are small joints at the back of your spine that guide and limit movement while helping stabilise the vertebrae. Like other joints, they can become irritated or arthritic over time. Degenerative change (“facet arthropathy”) is common with age and can contribute to lower back pain. (Radiopaedia)
What is lumbar facet joint pain?
“Facet pain” refers to pain thought to originate from the facet joints and surrounding structures. Studies suggest that in well-selected patients, facet joints account for a meaningful portion of non-specific low back pain—commonly quoted as ~15–45% depending on methods used (e.g., diagnostic blocks). (SpringerOpen)
Common causes & triggers
- Gradual wear and tear/osteoarthritis of the facet joints
- Periods of prolonged standing, extension (bending backwards), or repetitive twisting
- Postural/load changes, deconditioning, or a sudden increase in activity
- Occasionally after minor strains or with co-existing disc or muscular issues
Good news: for most people, conservative care (education, activity modification, and targeted exercise) is effective and preferred first-line management. (NICE, AAFP)
Typical symptoms (and how it differs from disc pain)
People with facet-mediated pain often report:
- Localised low back pain, sometimes felt off to one side
- Worse with extension (leaning backwards) and/or rotation
- Stiffness after sitting, improved with gentle movement
- Usually no leg symptoms below the knee (contrast with many disc irritation patterns)
Remember, symptoms overlap between conditions—your physio assessment is key to tailoring the right plan.
Do I need a scan?
Usually no to start with. Imaging often shows age-related changes that don’t perfectly match symptoms; routine scans are not recommended for most non-specific low back pain unless “red flags” are present. When indicated, particular diagnostic injections (medial branch blocks) can help confirm if the facet joint is the pain source—typically only after a trial of conservative care. (SpringerOpen, Europe PMC)
Seek urgent medical care if you have red flags such as: unexplained weight loss, fever, recent significant trauma, history of cancer, progressive neurological symptoms, or new bladder/bowel changes.
What actually helps? (Evidence-aligned care)
1) Keep moving (graded activity). Gentle mobility and a progressive exercise program reduce pain and improve function.
2) Targeted strengthening. We focus on trunk/postural endurance, hip strength, and movement control to reduce load on irritated joints.
3) Manual therapy (short-term). Hands-on techniques can settle symptoms enough to let you exercise more effectively.
4) Education & load management. Tweak your sitting/standing routine, break up long static postures, and pace heavier tasks.
5) Medications (short course, if needed). Your GP may advise simple analgesics; avoid long-term reliance.
Major guidelines (NICE; VA/DoD) emphasise exercise-centred care and generally de-emphasise routine injections for non-specific low back pain; interventional options may be considered only for well-selected, persistent cases after conservative care. (NICE, AAFP)
What about injections or radiofrequency ablation?
Facet/medial branch diagnostic blocks and radiofrequency ablation (RFA) can help some carefully selected people with persistent pain, particularly after 3+ months of evidence-based physio and lifestyle care. The evidence base is mixed and selection matters—talk to your GP/pain specialist if your symptoms persist despite doing the right basics. (BMJ Rapid Reports, Pain Physician)
Simple self-care tips you can start today
- Movement snacking: stand, walk, or perform 30–60 seconds of gentle mobility every 30–45 minutes of sitting.
- Neutral-ish spine under load: when carrying kids/shopping, hinge at hips and keep the load close.
- Alternate positions: sitting → standing desk → short walk cycles.
- Strength “minimums” (2–3×/week): bridges/hip hinge patterns, trunk endurance holds, and anti-rotation work.
- Sleep/support: if sore on waking, trial a small pillow under the waist/side-lying or between knees.
How LivFit Physio Mornington can help
At LivFit Physio Mornington (11 Railway Grove) we’ll:
- Perform a clear assessment (what’s driving your pain right now).
- Give you a personal plan (movement, strength, load tweaks).
- Provide hands-on care if helpful to settle symptoms.
- Progress you through home rehab or in-clinic gym rehab/Pilates to prevent recurrences.
- Coordinate with your GP if you need imaging, a medication review, or—if appropriate—discussion of interventional options.
Prefer to start at home? You can also trial our Level 1 Enzi program (intro exercises) before escalating.
When should I see a physio?
- Pain has lasted >2 weeks or keeps recurring
- Extension/twisting repeatedly flares your back
- You’re avoiding activity or worried about harming your back
- You want a plan that’s tailored to your life, job, and sport
Book an appointment: Online Bookings
Call: 03 5976 8447
Clinic: 11 Railway Grove, Mornington VIC 3931